Type 1 diabetes is an autoimmune disease in which the immune system attacks and destroys insulin-producing beta cells in the pancreas, resulting in insulin deficiency. Insulin is a hormone that regulates blood glucose levels and enables cells to use glucose for energy.
People with type 1 diabetes require daily insulin injections or an insulin pump to live as a result of this deficiency. They must also frequently check their blood sugar levels throughout the day to prevent complications such as hyperglycemia (high blood sugar) or hypoglycemia (low blood sugar). (low blood sugar). Type 1 diabetes usually manifests itself during infancy or adolescence, but it can strike at any age.
The precise cause of type 1 diabetes is unknown, but it is believed to be a combination of genetic and environmental factors. Type 1 diabetes differs from type 2 diabetes, which is characterized by a combination of insulin resistance and decreased insulin production and is frequently managed through lifestyle changes and medication.
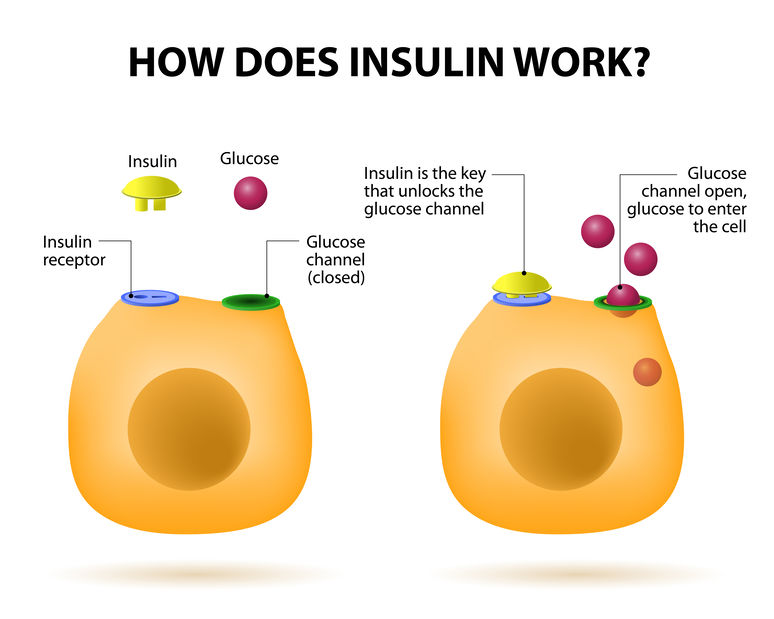
Insulin is a hormone that regulates the level of glucose in the bloodstream. It enables cells to absorb glucose and use it for energy or storage. Insulin is produced by the pancreas and is released in response to rising blood glucose levels. It then binds to insulin receptors on cells, signaling them to allow glucose to enter. This process helps to maintain normal blood sugar levels and provides energy for the body’s cells.
The CDC estimates 1.25 million Americans have type 1 diabetes. Managing a lifelong disease like diabetes in a child can be overwhelming, difficult, and frustrating, but being educated can help.
- Insulin deficiency causes type 1 diabetes. Cells get their energy from glucose, which is produced when people eat carbs. Insulin allows glucose use. Diabetes signs and complications result from blood glucose buildup due to insulin deficiency.
- Autoimmune type 1 diabetes lacks insulin. Diabetes auto-antibodies target insulin-producing cells. The cause is unclear. Genetics and environment are involved, according to research.
- Type 1 diabetes impacts everyone. Diabetics come from all ethnicities, but most are non-Hispanic white. 17,900 minors under 20 were diagnosed with type 1 diabetes in 2011–2012, according to the CDC. Diabetes can occur at any age, from infancy to middle age.
- Diabetes’ subtle symptoms grow over time. The kidneys clear glucose as glucose levels rise. Urination, thirst, and bedwetting rise. Fatigue, weight loss, and greater appetite result from glucose inefficiency. High glucose levels can cause life-threatening diabetic ketoacidosis (DKA), which causes vomiting, dehydration, and fatigue. This needs immediate medical attention.
- Laboratories diagnose type 1 diabetes. Visit a paediatrician or paediatric emergency room if you think your kid has diabetes. Doctors will check your child’s blood and pee glucose levels. They will also get a haemoglobin A1C test, which shows the three-month normal blood sugar. They may also test blood for type 1 diabetes autoantibodies.
- Insulin injections daily cure type 1 diabetes. After diagnosis, the kid is hospitalised for insulin therapy. Insulin needles are small and thin, unlike vaccination needles, which go into the muscle. Families are educated on insulin dosing, diet, exercise, sports, illness, and other daily life issues.
- No diet is “diabetic.” Healthy children receive similar nutritional advice. This includes a balance of carbohydrates, proteins, and healthy fats, having proper portions from each food group daily, and avoiding sugary foods. Diabetics should never skip meals and tally carbs in each meal.
- Teamwork manages diabetes. Complex diabetes care needs at least four annual visits with a diabetes care team. Doctors, nurses, diabetes educators, dietitians, social workers, and psychiatrists. The child’s personal support system is as essential as their diabetes management. Family, school aides, friends, significant others, and other carers can be part of the support and care team and receive training.
- Technology changes diabetes management. Researchers and experts worldwide have developed devices to better manage diabetes. Insulin units and CGMs are included. (CGMs). Pumps are discreet wearable devices that deliver insulin straight into the body. CGMs use Bluetooth to send real-time blood sugar levels to the wearer and family. Diabetes doctors recommend these devices for safety and efficiency.
- Control and good habits! Many teens and children with diabetes live full, healthy lives, play competitive sports, travel, and reach their goals. Nick Jonas, Gary Hall, Jr., Sonia Sotomayer, and Jay Cutler are famous diabetics. Diabetes care should fit into life, not vice versa. Carefully, this is doable.


